As a physician, I understand the profound and often debilitating impact that fibromyalgia can have on your daily life. The chronic, widespread pain, persistent fatigue, restless sleep, and cognitive difficulties—often referred to as “fibro fog”—can be incredibly challenging, affecting not just your physical well-being but also your emotional health and overall quality of life. While conventional medical treatments offer valuable tools for managing these symptoms, we often acknowledge their limitations in fully addressing the complex and multifaceted nature of this condition. Traditional pharmacotherapy, for instance, may not always provide complete relief, and some patients experience significant side effects, leading to an ongoing search for additional, more holistic support.
This is precisely why I want to discuss the increasingly vital role of complementary and alternative medicine (CAM) as an integral part of a comprehensive fibromyalgia care plan. Unlike approaches that primarily target individual symptoms, many CAM therapies embrace a holistic philosophy, aiming to restore balance and well-being across your entire system. This perspective, common in various traditional medicine systems worldwide, has a long history of successfully managing chronic conditions by addressing underlying imbalances rather than just surface symptoms.
The widespread interest in these therapies among our patients is striking; studies indicate that a remarkable 90% to 98% of individuals with fibromyalgia have explored CAM strategies to find relief. This high prevalence of use underscores the pressing need for effective, integrative solutions. We are seeing a growing body of evidence supporting the benefits of these approaches. For instance, systematic reviews have highlighted how therapies like homeopathy and certain herbal or dietary interventions can significantly improve pain at “tender points,” enhance sleep quality, and positively influence mood. Furthermore, practices such as meditation and acupuncture, have demonstrated particular promise in reducing pain, alleviating fatigue, mitigating sleep disturbances, and easing emotional rigidity.
While there are many steps you can take to reduce your risk or manage triggers for fibromyalgia, which you can read about here, in this article, we’ll explore together some complementary therapies that have shown promise in managing your condition. We’ll dive into the scientific evidence behind each one, helping you understand what the research suggests. My hope is that this information will empower you to discuss these approaches with your healthcare provider and potentially integrate beneficial options into your fibromyalgia treatment plan.
Natural compounds and supplements for Fibromyalgia Treatment
The exact causes of fibromyalgia are still a puzzle, which makes finding the right fibromyalgia treatment a journey for many. While we have conventional medical approaches, I know many of you are also curious about or already exploring complementary therapies, including herbal medicines and natural compounds. Let’s talk about some of these options and what the latest research tells us.
In fibromyalgia, your body’s pain processing system seems to be on overdrive. Growing evidence suggests that tiny powerhouses in our cells called mitochondria might not be working perfectly. This can lead to something called oxidative stress, an imbalance where harmful molecules called free radicals outweigh your body’s natural protectors (antioxidants). Additionally, certain proteins called pro-inflammatory cytokines can contribute to inflammation, further amplifying pain signals.
Many of the natural compounds we’ll discuss work by addressing these very issues. They often act as anti-inflammatory agents, calming down the body’s inflammatory responses, and as antioxidants, helping to neutralize those damaging free radicals. By bringing these systems back into balance, our hope is to reduce your pain and improve your overall well-being.
Now, let’s look at some commonly consumed compounds that have been studied for their effects on fibromyalgia symptoms. It’s important to remember that much of this research is still in its early stages, often conducted in labs or on animals, with a small number of human clinical trials available, but the findings are certainly promising and warrant taking into consideration.
Curcumin
The vibrant yellow spice, turmeric, contains a powerful active compound called curcumin. You might have heard about curcumin for its anti-inflammatory properties. Recent research is shedding light on how inflammation, particularly in the nervous system, plays a significant role in chronic pain conditions like fibromyalgia. Imagine your nervous system, especially the cells in your spinal cord called “glial cells” (microglia and astrocytes), becoming overly active or “fired up.” This “neuroinflammation” can contribute to the persistent pain and heightened sensitivity you experience. Scientists are increasingly interested in calming this neuroinflammation, and curcumin is a promising candidate being investigated for this very purpose.
Studies, both test tubes and animals’ studies, have shown that curcumin can significantly reduce the severity of neuroinflammation in chronic pain models. How does it do this? Curcumin appears to inhibit various pro-inflammatory signals within these glial cells. It essentially puts a brake on inflammatory cascades like the MAPK, NF-κβ, and JAK-STAT pathways, which are like domino effects that lead to inflammation. By impeding these pathways, curcumin reduces the release of inflammatory mediators, thereby decreasing pain hypersensitivity and spontaneous pain. What’s even more fascinating is that curcumin also seems to boost your body’s own natural anti-inflammatory agents, potentially functioning as an “immunomodulator” – helping to balance your immune response.
While the exact pathway by which curcumin exerts its main effect is still being investigated, growing evidence suggests it acts in multiple ways. Even if levels are low in the brain, curcumin can directly affect sensory neurons (nociceptors) that transmit pain signals. It does this by interacting with specific receptors, like TRPV1, purinergic receptors, and CX3CR1, in structures called the dorsal root ganglia. Beyond direct action, curcumin also influences peripheral immune cells and can even modulate your gut microbiota. These indirect actions are crucial because by managing inflammation in these peripheral areas, curcumin can potentially limit the activation of spinal glial cells, thereby reducing pain signals that travel to your central nervous system.
Now, here’s where it gets a bit tricky. Despite its promising effects, curcumin isn’t easily absorbed by the body. This “low bioavailability” means that a significant portion of orally administered curcumin doesn’t reach your bloodstream, let alone your brain, in sufficient concentrations to exert its full therapeutic potential. This is a major factor limiting its widespread use as a standalone therapy.
To overcome this, researchers are actively exploring strategies to improve curcumin’s absorption and delivery. This includes developing enhanced formulations like nanoparticles or combining curcumin with other compounds that boost its uptake. But we also need to be cautious. While curcumin generally has few side effects, increasing its absorption might lead to new challenges. Curcumin is a “polypharmacological” compound, meaning it interacts with many different targets in the body. If we increase its levels too much, it could have unintended effects. So, stick to the recommended doses, and as always, discuss with your physician before taking.
Omega-3 Fatty Acids
Omega-3 polyunsaturated fatty acids (PUFAs) are essential fats found abundantly in fish oil and certain plant-based oils. These fats are well-regarded for their ability to reduce inflammation throughout the body.

When it comes to fibromyalgia, human studies on omega-3 PUFA supplementation have yielded mixed, yet often encouraging, results. One clinical trial found that omega-3s can help reduce pain in tender points and improve overall function in individuals with fibromyalgia. However, their impact on other symptoms like mood and sleep disturbances has been less consistent. To truly understand their full benefits, we need more comprehensive human studies with larger participant groups, varied dosages, and longer treatment periods.
Ginger
Ginger is a staple in many kitchens and traditional medicine cabinets, valued for its potent anti-inflammatory and antioxidant compounds. These properties are key to its potential role in managing some of the inflammatory aspects that can accompany fibromyalgia.
While the research on ginger specifically for fibromyalgia is still emerging, studies generally indicate that compounds like ginger can reduce pro-inflammatory activity and increase antioxidant capacity in various cell types, including those found in our nerves and muscles. A 2018 animal study even suggests that daily consumption of ginger has been shown to improve several aspects of chronic pain, including sensitivity to touch and temperature, and an increased response to painful stimuli.
Beyond pain relief, GR also helps with behavioral changes often linked to chronic pain, such as problems with thinking, anxiety, and depression.
Notably, when ginger was given alongside paracetamol, the pain-relieving effects of paracetamol were significantly boosted.
These findings suggest that daily GR consumption not only enhances the pain-fighting effects of common pain relievers like paracetamol but also improves other thinking-related issues associated with long-term pain and reduces inflammation in conditions like fibromyalgia.
Enzyme Q10
When considering complementary approaches for fibromyalgia, many ask about Coenzyme Q10 (CoQ10), also known as ubiquinone. This compound is crucial for energy production in our cells. What’s particularly interesting for fibromyalgia is its potential role in addressing some of the underlying issues we see.
Research suggests that people with fibromyalgia often have lower levels of CoQ10. This is significant because CoQ10 may help with the inflammation, low antioxidant levels, and mitochondrial dysfunction that are thought to contribute to your symptoms. It appears to work by beneficially stimulating a gene called AMPK, which is involved in these processes. Studies have shown that supplementing with CoQ10, typically at doses of 300-400 mg/day, can help to replenish these levels and, importantly, reduce fibromyalgia symptoms, especially pain. Some research even suggests it can enhance the pain-relieving effects of medications like pregabalin. While more large-scale studies are needed, these initial findings are promising and offer a hopeful avenue for managing your pain.
Naringin
Naringin is a natural substance found in grapefruits and other citrus fruits. What’s particularly exciting about naringin, and its active form naringenin, is that it appears to have a good ability to get into the body and even cross into the brain. This is important because fibromyalgia involves the central nervous system.
Research, particularly in animal studies, suggests naringin may offer several benefits for fibromyalgia symptoms. One of its key actions is its anti-inflammatory effect. We know that inflammation can play a role in pain and other symptoms, and naringenin seems to help calm this process down. For instance, studies have shown it can reduce substances in the body that promote inflammation, which are often elevated in pain conditions.

Beyond inflammation, naringin also shows promise as an antioxidant and a neuroprotector. This means it can help protect your cells from damage and support the health of your nervous system. In animal models designed to mimic fibromyalgia, naringin has been shown to improve behaviors like anxiety and depression, increase social interaction, and even enhance cognitive performance.It seems to do this by improving communication between nerve cells and boosting the body’s natural defense systems against stress and damage.
Furthermore, studies indicate naringin can help with pain relief (what we call anti-nociceptive effects) across various types of pain. It may also combat fatigue, a common and debilitating symptom of fibromyalgia, by improving energy metabolism in the muscles. While these findings are largely from animal studies, they give us valuable insights into how naringin might work to ease the complex symptoms of fibromyalgia.
Grape Seed Extract
Grape seed extract (GSE), a natural plant derivative, is often a byproduct of winemaking. It’s packed with beneficial compounds called polyphenols, including things like proanthocyanidins and anthocyanins. These are powerful substances, and studies have shown GSE to have neuroprotective, antioxidant, and anti-inflammatory effects in lab and animal studies.
Now, let’s dive a bit deeper into how GSE might impact your fibromyalgia symptoms. Research suggests that the polyphenols in GSE may help decrease pain sensitivity. For instance, in animal models mimicking fibromyalgia, a specific type of proanthocyanidin called OPC (oligomeric proanthocyanidin complex) showed anti-hyperalgesic effects. This means it helped reduce the heightened pain response, likely because of its strong antioxidant and anti-inflammatory properties that can calm overactive pain pathways. Scientists even observed a decrease in a specific ion-sensing channel, ASIC3, which plays a role in pain signaling in the nervous system.
Beyond pain, fatigue is another major symptom. Animal studies have shown that GSE supplementation can actually increase fatigue threshold and extend the time to exhaustion in models of exercise-induced fatigue. This seems to happen by improving the body’s ability to cope with stress and by boosting important neurotransmitters like serotonin and noradrenaline, which play a role in energy levels and mood. Furthermore, GSE appeared to enhance the activity of enzymes vital for energy production in muscle cells and improve overall antioxidant capacity, which can combat the cellular stress contributing to fatigue.
While these mechanisms are being explored in animal studies, early human research provides a glimpse of potential benefits. One small trial on anthocyanins, a component of GSE, found that an 80 mg daily dose led to small but significant decreases in sleep disturbances and fatigue levels in patients with moderate to severe fibromyalgia over three months. This suggests a direct impact on these debilitating symptoms. While these findings are encouraging, it’s crucial to remember that more extensive human trials are needed to confirm these effects and determine the optimal dosage.
Research suggests that grape seed extract can help reduce pro-inflammatory activity and boost antioxidant capacity in cells and animal models. What’s particularly interesting is that grape seed extract, along with omega-3s, naringin, and genistein, seems to work in ways similar to some anti-seizure medications currently used for fibromyalgia. Beyond influencing nerve signals, these compounds offer the added benefit of protecting nerve cells (neuroprotection) and reducing inflammation in the nervous system, making them a very promising area of research.
Capsaicin
You might know capsaicin as the compound that gives chili peppers their kick. Beyond its culinary uses, capsaicin has been explored for its pain-relieving properties, particularly when applied topically to the skin.
Studies suggest that capsaicin can help reduce the production of inflammatory substances and boost the body’s natural antioxidant defenses within cells involved in pain regulation. For localized pain, some research has looked at using topical capsaicin cream. For instance, a pilot study examined its short-term effectiveness in patients with severe fibromyalgia, suggesting it might help lessen pain. Animal studies have also shown capsaicin can influence how sensitive we are to pain.
Genistein
Genistein is one of soy phytoestrogen isoflavones, which are compounds found abundantly in soy products. These natural substances, especially genistein and daidzein, act a bit like our body’s own estrogen, specifically binding to receptors in nerve and immune cells – areas crucial in fibromyalgia.
What’s exciting is how they might help with your symptoms. Animal studies suggest these compounds have pain-relieving, protective effects on nerves, and can even help balance the immune system and reduce inflammation. For instance, in models of fibromyalgia-like pain, genistein has been shown to reduce pain by influencing how pain signals are transmitted. It seems to work by calming down certain pain pathways involving “substance P,” a key player in sending pain messages, and by impacting nerve activity in the brain. Think of it as gently turning down the volume on some of the pain signals your body is sending. While these are promising findings from animal studies, they help us understand the potential mechanisms at play.
The research indicates that genistein, along with grape seed extract, omega-3s, and naringin, may function similarly to certain anticonvulsant medications used for fibromyalgia. Therefore, these substances hold great potential in safely managing the symptoms of fibromyalgia.
Vitamin D
A frequent connection between low vitamin D levels and chronic widespread pain, including fibromyalgia. This isn’t just a coincidence; there are some fascinating scientific reasons why these two might be linked.
The Pain Connection: Central Sensitization
One key theory is that vitamin D deficiency might contribute to what’s known as “central sensitization of pain processing.” Think of it like this: in someone with central sensitization, their nervous system becomes extra sensitive to pain signals. Even mild stimuli can feel intensely painful. We believe vitamin D plays a role in modulating these pain signals. This is because we find vitamin D receptors and enzymes that control vitamin D activity in areas of the body crucial for sensing and processing pain, such as your skin, spinal cord, and the nerves that carry pain messages.

Vitamin D as an Anti-Inflammatory Agent
Another exciting area of research suggests that vitamin D may have anti-inflammatory properties. Inflammation can certainly contribute to pain. Studies have shown that vitamin D might help reduce the production of certain inflammatory substances in the body, like prostaglandin E2 (PGE2). It can also influence immune cells, like macrophages and dendritic cells, encouraging them to produce fewer inflammatory chemicals and more anti-inflammatory ones. This suggests that when vitamin D levels are low, it might activate inflammatory pathways that contribute to both central and peripheral pain perception.
Lifestyle Factors and Vitamin D Levels
It’s also important to consider that the relationship can go both ways. Sometimes, the pain and fatigue associated with fibromyalgia can lead to lifestyle changes that inadvertently contribute to lower vitamin D levels. For instance, if you’re experiencing significant pain or depression, you might find yourself spending less time outdoors, which is where we get most of our natural vitamin D from sun exposure. Additionally, individuals with chronic pain conditions might tend to accumulate more fat mass. In those who are overweight, vitamin D can get “sequestered” or stored in fat tissue, making less of it available for your body to use. Interestingly, we’ve seen that weight loss can sometimes lead to an increase in circulating vitamin D levels, even without supplementation.
The Impact of Vitamin D Supplementation on Fibromyalgia Symptoms
So, what about taking vitamin D supplements? This is a question many patients ask. A recent comprehensive systematic review of many studies on this topic offers some valuable insights.
While some initial studies showed only limited pain relief with vitamin D supplementation, more robust research is emerging. Several high-quality studies suggests that appropriate vitamin D supplementation can have beneficial effects for individuals with chronic widespread pain, including fibromyalgia, especially if they have a confirmed vitamin D deficiency.
However, it’s important to understand that our understanding of the specifics is still being refined. For example, the ideal blood level of vitamin D (what we call the “25OHD threshold”) for treating fibromyalgia symptoms is still being studied. Similarly, the perfect dose, how often you should take it, and the best way to administer it (whether by mouth or injection) are areas where we need more clarity. While many studies have explored a dosage of 50,000 international units (IU) per week by mouth, we’re still working to determine the most effective and safest approach for everyone.
It’s crucial to remember that while raising vitamin D levels is generally beneficial if you’re deficient, taking very high doses, especially as a single annual dose, can sometimes have unexpected negative outcomes, such as liver injury or increased risk of falls and fractures in elderly women. This highlights the importance of working with your physician to determine the right dosage for you.
It’s also worth noting that simply having higher vitamin D levels doesn’t always translate to additional health benefits if you’re already at optimal levels. For instance, studies haven’t shown that vitamin D supplementation in individuals who are already vitamin D-replete (meaning their levels are fine) reduces the risk of cancer, cardiovascular events, hypertension, or type 2 diabetes. This emphasizes that supplementation is most beneficial for those who truly have suboptimal levels.
how can Chinese medicine be used in Fibromyalgia Treatment?
Many patients find themselves curious about herbal remedies and other TCM approaches, and for good reason – evidence-based studies in this area are growing, offering some promising insights. Some research reports that certain herbal preparations have shown real potential, sometimes even outperforming conventional medications in a number of studies.
What’s even more interesting is how herbal medicine can enhance other treatments. Imagine combining specific herbal formulations with your current medications, of course under your physician supervision. Research suggests this can lead to significantly greater pain reduction and an improved quality of life compared to using conventional medications alone. This suggests a synergistic effect, where the herbs and conventional medications work together to provide more comprehensive relief.
Acupuncture
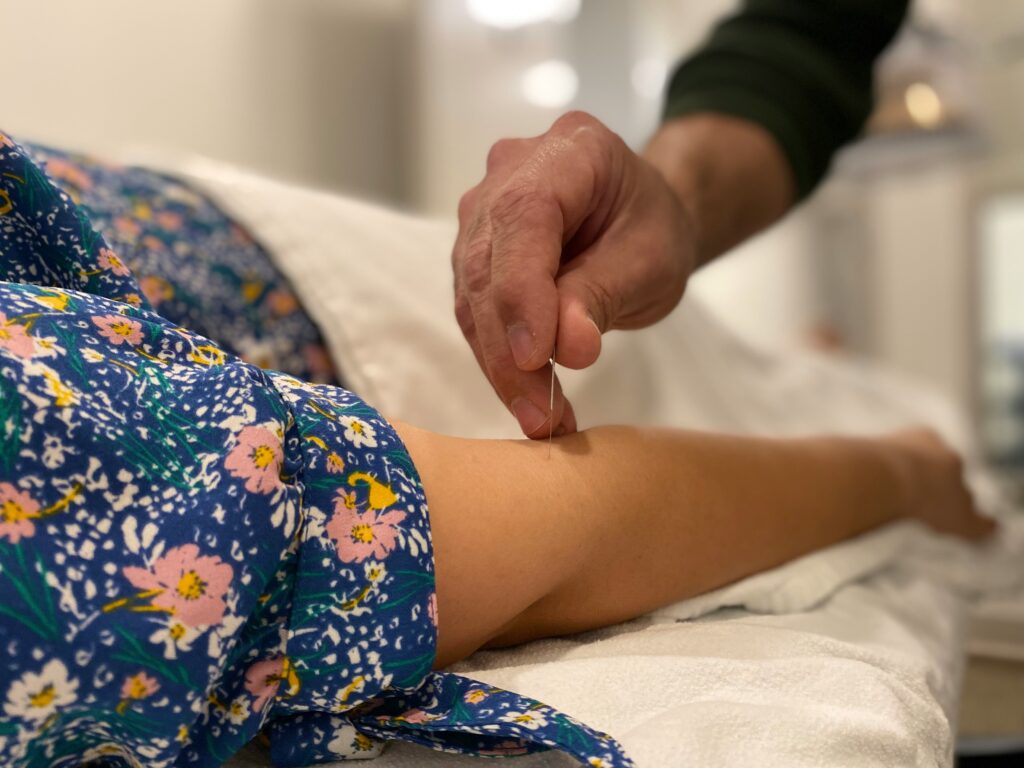
Acupuncture, an ancient practice from traditional Chinese medicine, involves precise needle placement at specific body points to restore balance to energy pathways, known as meridians, promoting natural healing and pain relief. For those with chronic pain conditions like fibromyalgia, acupuncture offers a distinct and promising avenue for symptom management. From a Western medical perspective, research suggests acupuncture may activate your body’s natural pain control systems, releasing beneficial compounds like endorphins and other neurotransmitters that modulate pain signals. It may also influence local blood flow and nerve conduction, contributing to its therapeutic effects.
Several systematic reviews and meta-analyses have highlighted encouraging results. One robust review, published in the Journal of Pain Research, found that acupuncture was significantly more effective than sham acupuncture in reducing pain intensity and improving overall quality of life for individuals with fibromyalgia. This positive impact was observed both in the short term and persisted in some long-term follow-up assessments, showing a measurable reduction in pain and notable improvement in quality-of-life scores. These studies generally reported a low to moderate quality of evidence, which is common in complex interventional studies and underscores the need for even larger, highly standardized trials.
The benefits of acupuncture for fibromyalgia appear to extend beyond just pain relief, with clinical trials indicating improvements in other distressing symptoms like sleep quality, stiffness, and related issues such as anxiety and depression. While evidence quality for these broader benefits varies, consistent reporting of improvements across different studies is encouraging. For instance, some research suggests acupuncture can help regulate levels of pain-modulating substances like serotonin and substance P, often imbalanced in fibromyalgia patients.
Acupuncture also boasts a favorable safety profile, with studies consistently reporting fewer side effects compared to many pharmacological fibromyalgia treatment. Any side effects are typically minor, such as slight bleeding or soreness. Given this safety, coupled with accumulating evidence of benefits, acupuncture is increasingly recommended as a valuable component of a multi-modal treatment plan for fibromyalgia, working synergistically with other approaches for comprehensive symptom management.
Hyperbaric oxygen therapy (HBOT) and Fibromyalgia Treatment
So, what exactly is hyperbaric oxygen therapy? Simply put, it’s a medical treatment where you breathe 100% pure oxygen in a special pressurized chamber. Think of it like a gentle dive, where the increased atmospheric pressure allows your body to absorb significantly more oxygen into your blood plasma than it normally would by breathing air at regular pressure. This “super-oxygenated” blood can then reach tissues throughout your body that might be struggling with low oxygen levels, promoting healing and reducing inflammation. While HBOT has been a long-standing treatment for conditions like decompression sickness and certain infections, its potential benefits for chronic conditions like fibromyalgia are now being rigorously explored.
How HBOT May Offer Relief in Fibromyalgia
The exact mechanisms by which HBOT helps alleviate fibromyalgia symptoms are still being investigated, but current research points to several promising pathways. One key theory revolves around addressing the issue of tissue hypoxia, or a lack of oxygen in various bodily tissues, which is thought to contribute to the pain and tenderness experienced by those with fibromyalgia. By dramatically increasing oxygen delivery, HBOT can help to correct this oxygen deficit, thereby fostering healing and reducing inflammation at a cellular level.
Furthermore, studies suggest that HBOT might promote neuroplasticity – essentially helping to “rewire” or reset pain pathways in the brain that have become overactive or dysfunctional in fibromyalgia. This enhanced oxygen delivery also appears to have anti-inflammatory effects and can help reduce oxidative stress, which are both believed to play a role in the chronic pain and other symptoms of fibromyalgia. It’s about optimizing your body’s innate healing capabilities.
Insights from Recent Studies
Let’s delve into some of the compelling findings from recent research that shed light on HBOT’s potential for fibromyalgia patients.
An important prospective clinical trial, provided early evidence suggesting that hyperbaric oxygen therapy can significantly diminish the symptoms of fibromyalgia syndrome. This study observed improvements in pain thresholds, physical functionality, and overall health-related quality of life. Patients undergoing HBOT also experienced a reduction in tender points – those specific spots that are often exquisitely painful for individuals with fibromyalgia – and a decrease in psychological distress. Interestingly, brain imaging in this study also revealed that abnormal brain activity patterns associated with fibromyalgia were normalized following HBOT, indicating a direct impact on the neurological underpinnings of the condition.
A more recent systematic review and meta-analysis, synthesized findings from multiple studies to provide a broader picture of HBOT’s efficacy and safety for fibromyalgia. This comprehensive analysis concluded that HBOT demonstrated lasting efficacy in treating core fibromyalgia symptoms, including pain, tenderness, fatigue, and sleep disturbances. The review highlighted HBOT’s strong anti-inflammatory potential and its ability to improve mitochondrial dysfunction in fibromyalgia patients, which is crucial for energy production within cells. By increasing pain thresholds, HBOT was shown to effectively reduce the number of tender points, breaking what can feel like a vicious cycle of pain and tissue hypoxia.
HBOT Versus Traditional Pharmacological Approaches
Perhaps one of the most exciting recent developments comes from a 2024 study published in, which directly compared HBOT with standard pharmacological care for individuals with fibromyalgia, particularly those with a history of childhood sexual abuse – a population that often experiences more severe and complex symptoms. The results were quite significant, revealing that HBOT offered superior benefits compared to medications in terms of physical, functional, and emotional improvements. Brain imaging further supported these findings, showing an increase in activity in specific pre-frontal and temporal brain areas in the HBOT group, which directly correlated with their symptom improvements. This suggests a powerful neuroplasticity effect of HBOT, helping to restore healthier brain function.
What This Means for You
These studies offer a beacon of hope for those navigating the complexities of fibromyalgia. While hyperbaric oxygen therapy is not yet a universally standard fibromyalgia treatment, the accumulating evidence is certainly compelling. So, I encourage you to view these findings as a valuable step forward in understanding more comprehensive treatment options.
It’s important to remember that HBOT, like any medical intervention, should be considered in consultation with your healthcare provider. And while generally well-tolerated, some individuals might experience mild, temporary side effects such as ear discomfort, similar to what you might feel during a plane ascent or descent.
The Lowdown
Living with fibromyalgia can be incredibly challenging, I fully understand the desire for effective, gentle treatments that can be used for long-term management of this condition without having to worry about the adverse effects that may occur with such chronic use. While conventional medicine has its place, many patients find significant relief by incorporating complementary therapies into their long-term care, often with fewer side effects than pharmaceutical treatments.
You may want to consider natural herbs and supplements, which can work with your body to reduce inflammation and manage pain without harsh reactions. Chinese medicine, including acupuncture, offers a holistic path to rebalance your system and address the root causes of symptoms. And Hyperbaric Oxygen Therapy (HBOT), has a great potential in managing the symptoms of this condition by increasing oxygen delivery, which been reported to significantly reduce pain and fatigue.
These approaches offer a powerful way to manage fibromyalgia, empowering you with options that support your body’s natural healing processes. And I hope this information can help you craft a comprehensive fibromyalgia treatment plan, with your healthcare team, that prioritizes your well-being, minimizes side effects, and ultimately, helps you live with less pain and more vitality.

